Responding to growing pressure – with ventilator shortfalls of over 500,000 being predicted, and states drawing up guidelines as to who should be left to die during ventilator shortages – the Food and Drug Administration [FDA] has finally begun to recommend the use of common CPAP and similar devices to help COVID-19 patients desperately needing help breathing.
Interestingly, one of the first to suggest such a strategy, and to widely publicize it, was an MIT-educated law professor, and inventor with several patents, who is best known for saving millions of lives by requiring broadcasters to air antismoking messages, and forcing cigarette commercials off radio and television.
The decision by the FDA to endorse and permit the use of CPAPs and similar devices – sometimes called “poor man’s ventilators – during the current coronavirus crisis is very important, says professor John Banzhaf, who is announcing the following FDA guidance dated March 22:
“Continuous Positive Airway Pressure (CPAP), auto-CPAP, and bilevel positive airway pressure (BiPAP or BPAP) machines typically used for treatment of sleep apnea (either in the home or facility setting) may be used to support patients with respiratory insufficiency provided appropriate monitoring (as available) and patient condition.”
CPAPs can help breathing for patients with moderate issues
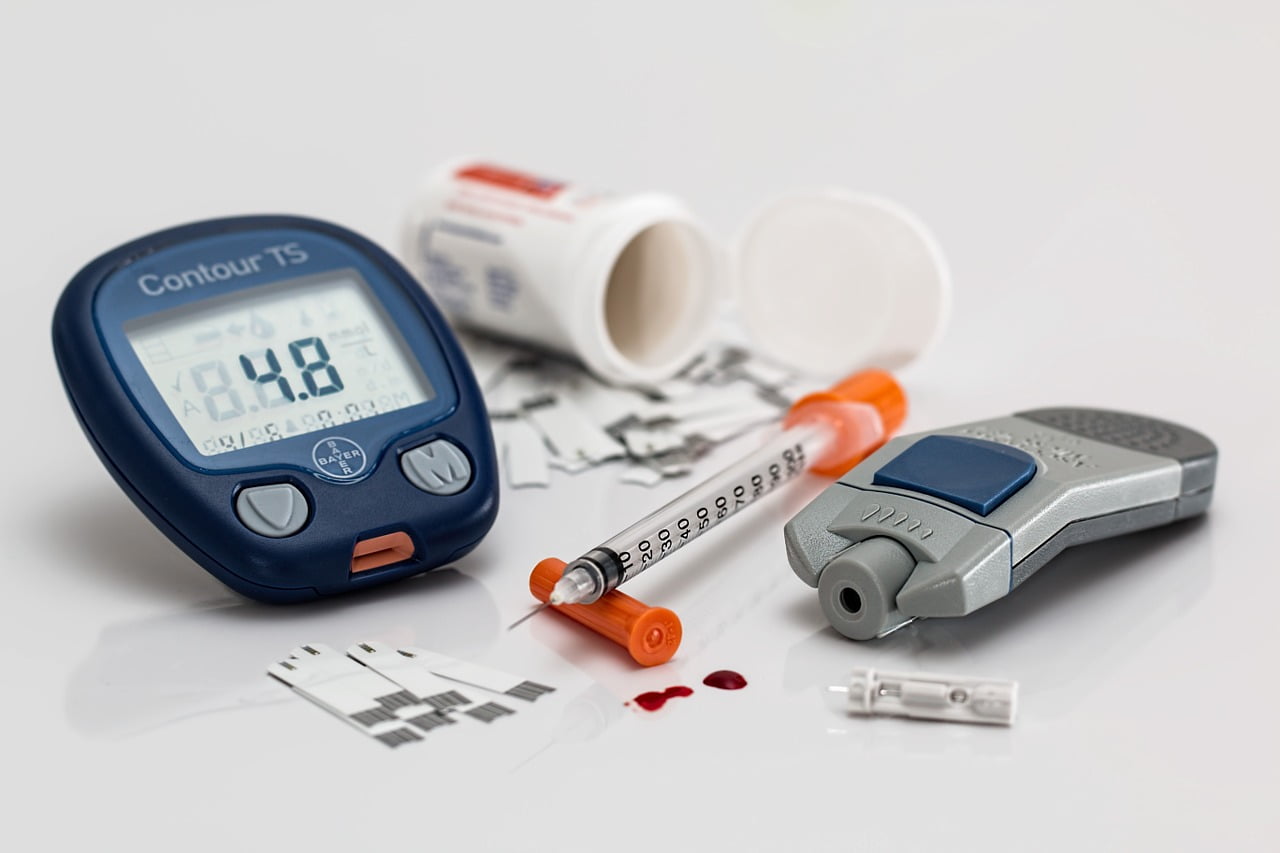
Banzhaf notes that, in contrast to medical ventilators (only about 160K now in hospitals), there are millions of CPAP and similar devices already in use, or in warehouses waiting to be used – to reduce snoring and treat sleep apnea (temporary periods of wakefulness) by helping to force air into the lungs of users – which may now be used to help hospitalized COVID-19 patients who require help breathing, but may not require the full power and sophistication of scarce and expensive ventilators.
In addition to those, many current users might be paid a nominal sum to do without their CPAP machines for a few months in situations where it would not create a serious health risk for them, and especially in cases where they have several older models left over from past use, or don’t regularly use their existing CPAP machine because it is uncomfortable, intrusive, inconvenient, not truly necessary, etc. Many have already agreed to do so, says Banzhaf.
Because they are much simpler to produce, and are currently made by many different companies, it is also much easier to increase CPAP production capacity to meet this extraordinary demand; something not true for hospital ventilator machines.
Moreover, at an average cost of only about $850 (and far less if purchased in bulk), hospitals would likely to be much more willing and able to purchase enough CPAPs to help meet the growing surge in demand than ventilators ($25,00-$50,000), especially since they would be able to sell or rent CPAPs thereafter to patients with sleep apnea and/or excessive snoring after the current crisis and the demand for so many ventilators drops.